Shocking Leak Reveals Why Your Knee Replacement Replacement Will Fail!
Have you ever wondered why some knee replacements fail despite modern medical advances? The truth is, knee replacement failure is more common than most patients realize, and understanding the reasons behind these failures could save you from unnecessary pain and multiple surgeries. This shocking revelation uncovers the hidden truths about why knee replacements fail and what you can do to prevent it.
Understanding Knee Replacement Surgery
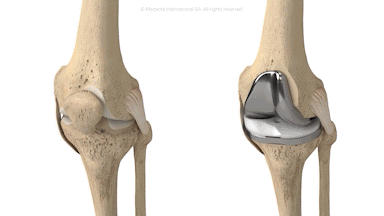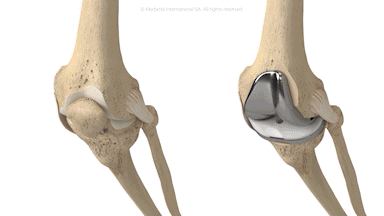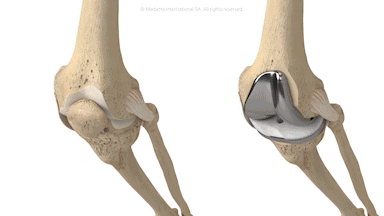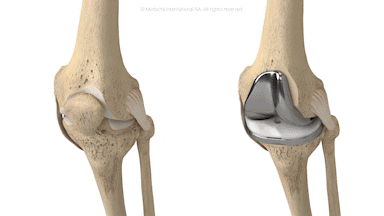
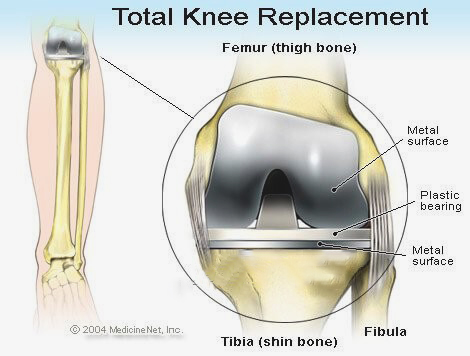
A knee replacement involves removing damaged surfaces of the femur (thigh bone) and the tibia (shin bone) and replacing them with artificial components. This surgical procedure has helped millions of people regain mobility and live pain-free lives. However, despite technological advancements, knee replacements don't always work as intended, and many patients find themselves facing unexpected complications.
The success of knee replacement surgery depends on multiple factors, including the patient's overall health, surgical technique, implant quality, and post-operative care. When any of these elements fail, the entire procedure can be compromised, leading to what's known as knee replacement failure.
- Pluribus Uncovered The Nude Scandal Behind Americas Motto
- The One Tea That Destroys Sore Throats In Minutes Shocking Discovery
- Kanye West Drops Bombshell Lyrics Saying Heil Hitler This Changes Everything
The Polyethylene Problem That Changed Everything
Polyethylene wear was once among the leading causes of knee replacement failure. The plastic liner that sits between the metal components of a knee implant absorbs the forces of daily movement. Over time, this polyethylene component would wear down, releasing tiny particles that could trigger an inflammatory response in the body.
As polyethylene production improved, modes of failure from polyethylene wear and subsequent osteolysis became less common. However, this improvement in one area revealed other vulnerabilities in knee replacement systems. The evolution of materials science in orthopedics has been a constant battle between durability and biocompatibility.
Modern polyethylene materials are now highly cross-linked and resistant to wear, but this advancement has shifted the focus to other potential failure mechanisms. Understanding this historical context helps explain why knee replacement failure patterns have changed over the decades.
- Ramon Rodriguez Sex Tape Scandal Shocking New Leak Exposes Everything
- Shocking Leak Los Dareyes De La Sierras Secret Sex Tape Exposed
- Ice Spices Body Transformation Exposed The Leaked Diet Plan That Changed Everything
Warning Signs of Knee Replacement Failure
Noticing signs of knee replacement failure like instability or new pain is crucial for early intervention. Patients should be aware that pain that returns months or years after successful surgery, swelling that doesn't subside, or a feeling that the knee is "giving way" could indicate serious problems with the implant.
Other warning signs include decreased range of motion, clicking or popping sounds from the knee, and warmth around the surgical site that persists. These symptoms shouldn't be ignored, as they often indicate that the implant is failing and needs immediate medical attention.
The timing of these symptoms can provide clues about the type of failure. Early failure (within weeks to months) often indicates surgical technique issues or infection, while late failure (years after surgery) typically points to wear, loosening, or osteolysis.
Why Implants Loosen and When Intervention Is Needed
We explain why implants loosen and when intervention is needed because this is one of the most common reasons for knee replacement failure. Aseptic loosening is a common reason, where the implant detaches from the bone without infection. This occurs when the bond between the implant and bone breaks down over time.
The loosening process typically begins with microscopic movements between the implant and bone. These movements create wear particles and stimulate the body's immune response, which ironically attacks the bone surrounding the implant. This process, called osteolysis, gradually destroys the bone and compromises the stability of the entire implant system.
Intervention is needed when conservative treatments fail to manage symptoms, or when imaging studies show significant loosening or bone loss. The decision to revise a failing knee replacement depends on the severity of symptoms, the extent of damage, and the patient's overall health status.
Historical Perspective on Total Knee Arthroplasty Failures
Historically, the most common mechanism of total knee arthroplasty (TKA) failures included aseptic loosening, instability and malalignment. These three factors accounted for the majority of revision surgeries performed in the early decades of knee replacement surgery.
As surgical techniques improved and implant designs became more sophisticated, the rates of these traditional failure modes decreased. However, this reduction in one type of failure often led to the emergence of new challenges. For instance, as surgeons became better at achieving proper alignment, issues related to soft tissue balance and kinematics became more apparent.
Understanding this historical progression helps both patients and surgeons set realistic expectations about knee replacement longevity and potential complications. It also highlights the ongoing nature of innovation in joint replacement surgery.
Primary Causes of Knee Replacement Failure
Primary causes of knee replacement failure several factors can lead to knee replacement failure, ranging from mechanical issues to biological responses. Beyond the well-known causes like polyethylene wear and aseptic loosening, other factors include infection, component malpositioning, and patient-specific factors such as obesity or high-impact activities.
Infection remains one of the most serious complications, potentially requiring complete removal of the implant and prolonged antibiotic treatment. Even when successfully treated, infection can significantly compromise the bone stock and soft tissues, making future revisions more challenging.
Component malpositioning, whether due to surgical error or implant design limitations, can lead to accelerated wear, instability, and patient dissatisfaction. Modern surgical navigation and robotic-assisted techniques have helped reduce these errors, but they remain a concern.
The Complex Anatomy of the Knee Joint
The knee has circumferential attachments between the tibia and femur and only releasing the main ligaments on the sides unfortunately is incomplete. This anatomical reality is crucial for understanding why some knee replacements fail to restore normal function. The knee is not simply a hinge joint but a complex structure with multiple degrees of freedom.
The cruciate ligaments, collateral ligaments, and surrounding soft tissues all contribute to knee stability and function. When a total knee replacement is performed, some of these structures must be sacrificed or significantly altered. The challenge for surgeons is to recreate stability and motion using the remaining anatomy and the prosthetic components.
This complexity explains why achieving perfect knee kinematics with a replacement is so challenging. Even the best-designed implants cannot fully replicate the intricate movements and force distributions of a healthy, natural knee joint.
The Myth of Single Radius Knee Design
The idea that only 2 main ligaments create the bend direction or radius of bend/flexion refers to a 'single radius' idea of knee replacement. This simplified model of knee motion has influenced implant design for decades, but it fails to capture the true complexity of knee biomechanics.
Modern understanding recognizes that the knee moves through multiple radii during flexion and extension, and that these movements are influenced by the complex interactions between bones, ligaments, and soft tissues. Single-radius designs, while easier to manufacture and sometimes easier to balance surgically, may not provide the most natural feeling knee motion.
This realization has led to the development of multi-radius and asymmetrical designs that attempt to better mimic natural knee kinematics. However, the debate continues about whether these more complex designs provide meaningful clinical benefits over simpler designs.
Replacement Information Sheet: Why Knee Replacements Fail
Replacement information sheet why knee replacements fail needs to address both patient and surgeon perspectives. From the patient's viewpoint, understanding the reasons for failure can help in making informed decisions about surgery and post-operative care. From the surgeon's perspective, this knowledge guides surgical technique and implant selection.
Common failure mechanisms include:
- Aseptic loosening due to osteolysis
- Polyethylene wear and debris generation
- Infection (early or late)
- Instability due to soft tissue imbalance
- Component malpositioning or malalignment
- Trauma or high-impact activities
- Patient factors (obesity, osteoporosis, poor compliance)
Each of these mechanisms has specific risk factors and may require different approaches to prevention or treatment. Comprehensive patient education about these risks is essential for informed consent and optimal outcomes.
The Promise and Reality of Total Knee Replacement
Causes, warning signs, and prevention tips total knee replacement often provides significant pain relief and restores mobility in patients with severely damaged joints. Thanks to this intervention, millions of people experience significant improvement in their quality of life. The success stories are numerous and genuinely life-changing for many patients.
However, the reality is that total knee replacement is not a guaranteed permanent solution. While many implants last 15-20 years or longer, a significant percentage of patients will require revision surgery at some point. The challenge for both patients and surgeons is to maximize the lifespan of the initial replacement while being prepared for the possibility of future interventions.
Understanding both the benefits and limitations of total knee replacement allows for realistic expectations and better long-term outcomes. This balanced perspective is crucial for patient satisfaction and optimal utilization of healthcare resources.
Phantom Limb Pain: A Different Kind of Post-Surgical Pain
Phantom limb pain occurs after an amputation. You feel real pain in the part of the limb that's missing. Treatment is available to manage it. While this phenomenon is more commonly associated with major limb amputations, some knee replacement patients report similar sensations.
This type of pain is believed to result from the brain's attempt to reconcile the loss of sensory input from the removed joint structures. The nervous system may continue to send pain signals to a joint that is no longer anatomically present, creating a confusing and often distressing experience for patients.
Treatment approaches for phantom pain after knee replacement may include medications, nerve blocks, physical therapy, and psychological interventions. Recognition of this phenomenon by both patients and healthcare providers is important for appropriate management and improved quality of life.
The Importance of Surveillance and Early Detection
We try to expose and catch as many as we can when it comes to early signs of knee replacement failure. Regular follow-up appointments, including physical examinations and imaging studies, are essential for detecting problems before they become severe enough to cause significant symptoms or irreversible damage.
Surveillance protocols typically include annual or biennial X-rays, and more frequent imaging if symptoms develop. Advanced imaging techniques like CT scans or MRI may be needed to evaluate specific concerns such as loosening, osteolysis, or component positioning.
Early detection allows for intervention at a stage when less invasive treatments might be effective, or when revision surgery, if needed, is likely to be less complex and have better outcomes. This proactive approach to joint replacement care is a key factor in maximizing implant longevity.
When Your Knee Replacement Needs Replacement
How do you know when you need to get your knee replacement replaced? This question troubles many patients who have had successful surgery for years but are now experiencing new symptoms. The decision to proceed with revision surgery is complex and must balance the risks of additional surgery against the consequences of leaving a failing implant in place.
Key indicators for revision include:
- Persistent pain that limits activities and doesn't respond to conservative treatment
- Significant functional decline or instability
- Progressive loosening shown on imaging studies
- Recurrent infection that cannot be controlled
- Severe polyethylene wear with associated bone loss
The decision-making process should involve thorough discussion between the patient, surgeon, and often a multidisciplinary team. Factors such as the patient's age, activity level, overall health, and personal preferences all play important roles in this decision.
Understanding Knee Revision Surgery
Learn more about knee revision surgery and getting your knee prostheses exchanged. Revision surgery is inherently more complex than primary replacement due to factors like reduced bone stock, altered anatomy, scar tissue, and the technical challenges of removing well-fixed implants.
The goals of revision surgery include relieving pain, restoring function, and addressing the underlying cause of failure. However, the outcomes of revision surgery are generally not as predictable or consistently excellent as primary replacements. Patients should understand that while revision can provide significant improvement, it may not fully restore the function achieved with the original surgery.
Modern revision techniques and implants have improved outcomes, but the procedure remains challenging. Careful patient selection and meticulous surgical technique are essential for successful revision surgery.
Conclusion
Understanding why knee replacement replacements fail is crucial for both patients and healthcare providers. From polyethylene wear and aseptic loosening to complex anatomical considerations and the challenges of revision surgery, the factors contributing to implant failure are numerous and interconnected.
The shocking truth is that no knee replacement lasts forever, and being prepared for this possibility is part of responsible joint replacement care. However, this shouldn't overshadow the tremendous benefits that knee replacement provides for millions of people worldwide.
By understanding the warning signs, maintaining regular surveillance, and making informed decisions about revision when necessary, patients can maximize the benefits of their knee replacement while minimizing the risks of failure. The future of joint replacement continues to evolve, with new materials, designs, and techniques promising even better outcomes for future generations of patients.
Remember, your joint replacement journey doesn't end with the initial surgery. It's an ongoing process that requires partnership between you and your healthcare team to ensure the best possible long-term results. Stay informed, stay vigilant, and don't hesitate to seek evaluation if you have concerns about your knee replacement's performance.